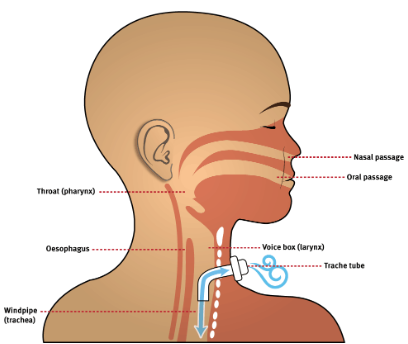
A tracheostomy tube is inserted into the windpipe (trachea) through a surgically created hole in the neck called a stoma. The operation to make the stoma is called a tracheotomy.
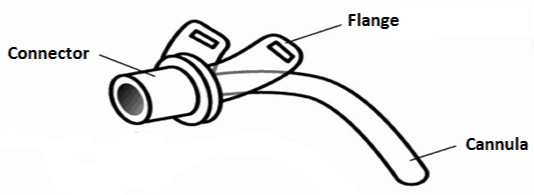
The tube includes a:
- cannula – this sits inside your child’s trachea
- connector or hub – this sits out from your child’s neck and is where you put the suction catheter to remove secretions
- neck plate or flange – these look like wings that sit against the neck.
Some tubes also have a balloon around the cannula inside the airway, called a cuff. This stops saliva and secretions from going in. This is usually only for older children.
Why does my child need a tube?
Your child may need a tube if their breathing nerves or muscles don’t work properly.
They may also need one if they:
- have a condition that makes them get tired easily
- have problems in their airway, head or neck that makes it hard for them to breathe
- have a condition that affects the shape of parts of their head and neck
- can’t swallow their saliva
- produce excess secretions that are difficult to clear from their chest.
Benefits of a tube
The benefits include:
- breathing easier
- having clear airways
- improved health, growth and development.
Challenges of a tube
Some of the challenges include:
- trouble eating and drinking
- sensitivity around the mouth, gagging and coughing with meals and not wanting to eat
- food or fluid going into the airway
- difficulties speaking – your child may need to use gestures or signs, picture boards or other forms of communication or a speaking valve
- not being able to swim.
Removal of the tracheostomy tube
Your child can have their tracheostomy tube removed when they no longer have airway problems.
To have the tube removed, your child will need to go to hospital. Your medical team will let you know when this can happen.
Developed by the Speech Pathology Department, Queensland Children’s Hospital. We acknowledge the input of consumers and carers.
Developed by the Speech Pathology Department, Queensland Children’s Hospital. We acknowledge the input of consumers and carers.
Resource ID: FS287. Reviewed: June 2023.
Disclaimer: This information has been produced by healthcare professionals as a guideline only and is intended to support, not replace, discussion with your child’s doctor or healthcare professionals. Information is updated regularly, so please check you are referring to the most recent version. Seek medical advice, as appropriate, for concerns regarding your child’s health.
Last updated: October 2023