Pressure injuries (also known as pressure sores or bed sores) can develop on the skin and underlying tissue when there is constant pressure or friction. Pressure injuries can develop quickly, especially when your child is unwell. Regular position changes, checking your child’s skin, good hygiene and skin care, and a healthy diet can all help prevent pressure injuries from forming.
Where do they occur?
Pressure injuries can occur anywhere on a child’s body when they are spending long periods of time in bed or a wheelchair. They are especially likely to appear on the bony parts of the body such as heels, elbows, hips, buttocks, tailbone, nose, ears, and the back of the head. They can also develop anywhere a medical device is touching your child’s skin, such as a tube, cast, splint, drip, drain or monitoring attachment.
Pressure injuries can present as changes in skin colour (red, blue or purple), like a bruise, or as damage to the skin (such as a blister or open wound). The images below are examples of what a pressure injury looks like when it first starts to form (stage 1), and when it progresses further (stage 2).
Stage 1
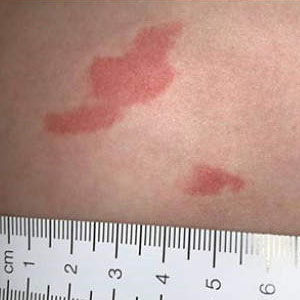
Stage 2
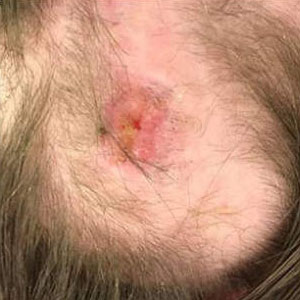
Things you can do to help prevent pressure injuries
It can be helpful to talk to your child’s nurse about developing a plan for preventing pressure injuries. It can also help to:
- Be involved in checking your child’s skin at least once a day. If you find an area with redness or a mark, speak with your child’s care team or nurse about ways to relieve the pressure.
- Change your child’s position regularly if they are unable to move themselves – aim for every two hours during the day, and every four hours at night. If your child can move by themselves, encourage them to change their position regularly if they are sitting or in bed for long periods of time.
- Make sure your child is getting food and fluids that are right for them.
- If your child is wearing nappies or continence aids, make sure to change them as soon as they are soiled.
- Immediately notify the nurse of foul-smelling odours under casts or splints.
- Avoid massaging reddened or bony areas of your child’s body, as pulling or stretching the skin may cause more damage.
Please note: In the Paediatric Intensive Care Unit (PICU) there will be extra equipment and devices attached to your child because they are critically unwell. This equipment is vital to your child’s care and should be handled carefully. Your bedside nurse will guide you on how to safely prevent pressure injuries where this equipment touches your child’s skin.
Tell your child’s care team immediately
- If you notice anything abnormal about your child’s skin
- If your child complains of pain or soreness, discomfort or pins and needles
- If your child complains of pain around an attachment or device or under a splint or cast
In an emergency, call Triple Zero (000) and ask for an ambulance.
If you're not sure whether to go to an emergency department, call 13 HEALTH (13 43 25 84) and speak to a registered nurse.
Developed by Patient Safety and Quality Service, Queensland Children’s Hospital. We acknowledge the input of consumers and carers.
Resource ID: FS162. Reviewed: June 2020.
Disclaimer: This information has been produced by healthcare professionals as a guideline only and is intended to support, not replace, discussion with your child’s doctor or healthcare professionals. Information is updated regularly, so please check you are referring to the most recent version. Seek medical advice, as appropriate, for concerns regarding your child’s health.